Pregnancy-related low back pain (LBP) and pelvic girdle pain (PGP) have been associated with an alteration in the strategy for lumbopelvic stabilization. Different core stabilization approaches exist, the evidence is however controversial.
MethodsThis paper discusses how to improve the evidence of exercises for women suffering from LBP and PGP during and after pregnancy. Exercises should be understood in a context, where the bio-psycho-social perspective directs the prescription of exercises, targeting both psychological and physical factors. The type of exercise probably should be individually tailored to the needs and capability of the individual and it is not only about the most appropriate exercise, it is about dosage and delivery of the exercises, and it is about performance. To promote adherence the use of patient preferences, with self-defined movement goals, may be a motivational basis for behavior change. Communication skills may facilitate positive beliefs and provide a motivational foundation for empowerment, self-efficacy and for self-management. To learn by discovery where the patient learns through their own experiences, might motivate the patients to active engagement and to behavioral change. Adherence probably will increase when the patients understand the aim and the rationale behind the exercises they are prescribed. However, with high adherence to exercises that maintains an inappropriate motor pattern, LBP and PGP possibly could proceed into chronicity.
ConclusionExercises need to be meaningful to the patient, relevant for daily activities, individualized according to patient preferences, guided and supervised to secure performance and quality.
Women with low back pain (LBP) and pelvic girdle pain (PGP) report a significantly lower health-related quality of life than that reported by healthy women.1,2 A major factor affecting the women's quality of life is lack of physical ability and a greater loss of physical condition seems to be not a cause but rather a consequence of LBP and PGP in pregnancy.3 Although exercise is recommended during pregnancy, pregnant women are tending to reduce their levels of physical activity.4,5 Whereas most women recover after delivery, a number of women continue living with disabling PGP for months and years. Discouragement, isolation and loneliness may be part of women's lives with pain and limited physical activity.6
LBP is usually defined as pain between the twelfth rib and the gluteal fold,7 whereas PGP is defined as pain experienced between the posterior iliac crest and the gluteal fold, particularly in the vicinity of the sacroiliac joints.8 Even though similar and overlapping features may be ascribed to LBP and to PGP, it is maintained that a distinction should be made.8,9 PGP generally arises in relation to pregnancy and is reported to be the most common condition, affecting 50% of the symptomatic patients. LBP affects about one-third and one-sixth report PGP and LBP combined.10 Women with PGP experience more intense pain and greater disability than women with LBP in pregnancy.11,12
The etiology and pathogenesis of PGP is unclear and probably multifactorial, including psychosocial factors. Underlying causes may include hormonal and biomechanical aspects, inadequate motor control and stress on ligament structures.13 Increased shear forces across the pelvic joints have been suggested to be one factor for pain in women with PGP.8 The pelvis serves to transfer load from the trunk to the legs, and for the load to be effectively transferred and for the shear forces to be minimized across the joints, the pelvis needs to be stabilized. An impaired load transfer during activities may result in overload of the ligaments of the pelvis and hence have an influence on PGP.14,15 Changes in spinal curvature and posture may be caused by pregnancy and both increased lumbar lordosis16 and a flattening of the lumbar spine or a lumbar kyphosis is reported to be prevalent during pregnancy.17,18 Frequent or sustained pain-provoking postures and movements might influence the pelvic ligaments and in turn link to other symptoms.
PGP have been associated with an alteration in the strategy for lumbopelvic stabilization with insufficient as well as excessive motor activation of the lumbopelvic and surrounding musculature.19 Hence, impaired motor control patterns may be a possible mechanism for ongoing pain and disability in patients with persistent PGP.20 Also, positive changes in motor control have been found to be associated with relief of pain and disability.21,22 While the role of muscle function in LBP in the general population is debated, an association between reduced muscle function and LBP and/or PGP in pregnant women is reported.23 In pregnant women with LBP and/or PGP, both lower levels of trunk muscle endurance and hip extension muscle strength24 and increased muscle activity during the active straight leg raise test are reported.25 Consequently, an association between muscle dysfunction and LBP and PGP during and after pregnancy may exist.
Specific exercises for motor control and stability have been recommended for PGP postpartum.8 The level of evidence is, however, limited, as few randomized controlled trials have been performed. The effectiveness of motor control and stability exercises for the treatment of LBP and PGP postpartum has been investigated in one systematic review.26 Different interventions were compared and with no firm conclusion of evidence.22,27–29 Also, group fitness classes for pregnant women showed in a randomized controlled trial no effect on the prevalence of LBP and PGP during pregnancy or postpartum.30
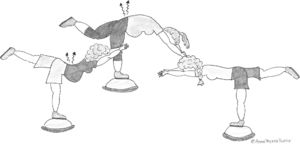
Despite limited evidence of effect, core stabilization exercises have grown in popularity31 and different core stabilization approaches exist.32,33 Exercises on unstable surfaces, as illustrated in Fig. 1, is an example of a stabilizing exercise commonly used and prescribed for LBP and PGP in many countries over the last years. We may however question: Why are patients recommended such exercises? What is the aim of the exercise? Does it help for LBP and PGP? What about the quality of the exercise? Does performance matter? Furthermore, do patients adhere to such exercises and will adherence to exercises be sufficient for reducing LBP and PGP? Finally, what about the evidence?
ExercisesEvidence of exercisesExercise may be defined as physical activity that is planned, structured, and repetitive for the purpose of conditioning any part of the body. Exercise is used to improve health, maintain fitness and is important as a means of physical rehabilitation.34 Supervised exercise therapy has been recommended as first-line treatment for chronic LBP the last 10 years.35 Still, evidence show that exercise therapy only has moderate effect on LBP, no clear evidence of effect on PGP, and it seems like one form of exercise is not superior to other forms of exercises.36–41 However, the last decade stabilizing exercises or motor control exercises has blamed over us worldwide as the choice of optimal exercises for LBP and PGP. Stabilizing exercises has been referred to as exercise interventions that aim to improve function of specific trunk muscles thought to control inter-segmental movement of the spine and enable the patient to regain control and coordination of the spine and pelvis using principles of motor learning.42 Core stabilizing exercises has for years been the focus for researchers, fitness centers, patients and for clinicians. Although stabilizing exercises have become very popular, the evidence is controversial. Some recent reviews conclude that stabilization exercises are more effective than general exercise, while others state the opposite.43–46 Hence, even core stabilization exercises do not give convincing evidence of effect. However, an agreed definition of core stabilization exercises does not exist.
Aim of the exerciseThe internationally endorsed Consensus on Exercise Reporting Template (CERT) is a 16-item checklist to improve the reporting of exercise programs and hopefully also the design and implementation of exercise programs.47,48 The CERT has recently shown to have good inter-rater agreement and to comprehensively evaluate reporting of exercise interventions.49 The checklist contains the following 7 categories: materials (what), provider (who), delivery (how), location (where), dosage (when, how much), tailoring (what, how) and compliance (how well/planned and actual). However, as commented by the authors of the CERT an explicit statement of the aim of the exercise, ‘why’ is missing.50 The aim of an exercise probably will influence on the design and the outcomes of an exercise intervention, and the aim of the exercise might be of significant importance for the patient's motivation and hence on adherence.
Consequently, what are the aim and the relevance of stabilizing exercises standing on unstable surfaces? An exercise standing on unstable surfaces, such as in Fig. 1, could be labeled a stabilizing exercise or a motor control exercise. Definitely, subjects standing on unstable surfaces have to activate muscles not to fall off, but is it necessarily an optimal motor control exercise? Could the performance of the exercise be maladaptive to the women's pain behaviors and complaints? Increased co-contraction with hyperactivity of core muscles and excessively guarded spinal movement with inability to relax spinal muscles are reported among LBP patients.51,52 Hence, the value of core stability exercises that promote bracing or excessively increasing trunk muscle activation could be questioned.53 It could also be questioned whether the women illustrated in Fig. 1 are doing the same exercise with similar motor pattern and similar to what is shown by the instructor? Or is it likely that they use different motor patterns? If increased activity of the extensor muscles and a lumbar lordosis increase the LBP for a woman, would we expect an exercise where this motor pattern is maintained, to reduce the woman's LBP? Opposite, if a flexion pattern provokes PGP for a woman will an exercise where she sustains a flexion pattern be a good exercise for her PGP? Probably not.
There is a lack of evidence linking the effects of exercise in LBP to changes in the musculoskeletal system,54,55 but performance of an exercise may result in increased pain or in persistence of pain.56 Quality and performance of exercises are considered as important aspects in reducing LBP and PGP.48,57 Inappropriate exercise can do more harm than good, with the definition of inappropriate varying according to the individual. Subsequently, what about high adherence to inappropriate exercises? It might be that the women stop exercising because they do not understand why they should do the exercise or because it does not reduce their LBP and PGP? And maybe they should be advised to stop, because the exercise maintains their inappropriate motor pattern. Stabilizing exercises could also create negative cognitions about instability and increase fear-avoidance.50
Individualization and adherenceExercises should be understood in a context, where the bio-psycho-social perspective guides the prescription of exercises, targeting both psychological and physical factors.58 The type of exercise probably should be individually tailored to the needs and abilities of the individual, and it is not only about the most appropriate exercise, it's about dosage (frequency, duration, intensity) and delivery (group, individualized, home-based) of the exercises.36,40,48 And it's about quality (performance, supervision) of the exercise, how are the exercises performed, do the patient need to be supervised?
One randomized controlled trial has shown significant and long-lasting positive effects of a treatment program for postpartum PGP, including stabilizing exercises.2,22 Why did this study show positive effects? This was an individualized and multidimensional treatment program focusing motor control and functional exercises, and necessarily integrated cognitive aspects within a bio-psycho-social framework. The exercises focused gradually progression of motor control and strength, performed without provoking pain, which has been shown to be important for adherence.59 Furthermore, the aim of the exercises had a functional approach based on the women's needs. The women learned to normalize pain provocative daily life activities, postures and movements to avoid flare-ups of pain.
The exercises were individualized and supervised. The aim of the exercise was clear to the patient (whether it was about control, strength or endurance), and performance (how) with relaxation to avoid muscle guarding was emphasized. An exercise diary was used for dosage and to show progression; consequently to increase motivation and adherence, and adherence was surprisingly high. Despite a busy life taking care of children, suffering from persistent pain postpartum, the women reported accomplishing on average 80% of their home based exercise program. And why was that? Adherence is very much about the way the exercises are provided.60 To promote adherence the use of patient preferences, with self-defined movement goals, may be a motivational basis for behavior change.53,60 Other important components are implementation (individually designed, supervised, home based exercises) and performance feedback (correcting movement patterns). Furthermore, communication skills may facilitate positive beliefs and provide a motivational foundation for empowerment, self-efficacy and for self-management and empowerment.61–63
The updated LBP guidelines from the National Institute for Health and Care Excellence (NICE) show a clear emphasis on facilitating self-management strategies.64 The guideline suggests that patient's needs, preferences and capability should be taken into account. It is of significant importance that health care providers not consider themselves as experts or teachers and consider the patients as ‘empty bottles’. Learning by Discovery65,66 encourages active engagement, promotes motivation, and promotes autonomy, responsibility and independence. It develops creativity and problem solving skills and tailoring learning experiences. To learn by discovery hopefully will motivate the patients to active engagement and to behavioral change. The patient learns through their own experiences. For example when a patient reports pain while standing, guiding them to change position and then question if the change influenced on their pain, and if it did, the patient discovers a difference, which probably will motivate them to perform changes during daily life and while performing exercises. In other words, the design of an exercise program probably will influence on program effectiveness.
Design of exercise studiesToday there is a wide variation among studies in how exercises are named and implemented and because most trials do not adequately report intervention details, information can be difficult to obtain.49 When comparing exercise therapy, we might question why studies show controversial results? It could be, because we are comparing ‘apples and pears’? In a study by Macedo et al.,38 it is shown that two studies, by O'Sullivan et al.67 and Stuge et al.,2,22 showed significant and long-term effect of an exercise intervention. What do these two studies have in common? First of all, they included sub-groups of LBP and PGP. Both studies also focused individual exercises incorporated into functionally daily life activities that commonly aggravated the patients’ symptoms, and the exercises were supervised and delivered as home exercises on daily basis.
It has been shown that therapy that is specifically directed at well-defined sub-groups leads to improved effectiveness of interventions.68 Lumping heterogeneous LBP and PGP patients into an exercise study will help in getting sufficient power for the study, but will a “one-size-fits-all” approach be optimal treatment for the individual patient?68,69 It could be questioned whether unidimensional care such as a “stay active” approach will target underlying mechanisms of LBP and PGP? The most effective exercise therapy to improve pain and function in chronic LBP has shown to be individually designed treatment programs that were supervised and delivered as home exercise with regular therapist follow-up to encourage adherence.36 Adherence probably will increase when the patients understand the aim and the rationale behind the individual exercise they are prescribed, but are adherence enough?
With high adherence to exercises that maintains an inappropriate motor pattern, LBP and PGP possibly could proceed into chronicity. Exercises might be labeled motor control exercises, but with an inappropriate performance it may result in stiffness and rigidity, quite commonly seen in patients doing stabilizing exercises. Increased co-contraction of trunk stabilizing muscles during tasks that provoke pain and an inability to relax muscles are reported in both LBP and in PGP.70,71 The exercises may be more about strength than about motor control. Patients may comply with their prescribed exercises; they get strong, but also stiff and rigid and with no improvement in pain and function. Neuromuscular control or core stability is needed to perform daily life activities, but only low levels of muscle contraction are needed to stabilize the spine.72 So, when are patients strong enough? Is it a good choice to continue doing the same exercises when the exercises do not reduce LBP and PGP? Furthermore, which muscles do we need to strengthen?
Bending and lifting are daily functional activities which may be challenging for patients with LBP and PGP. The quadriceps muscle was paid attention to years ago where rehabilitation of low-back-injured workers focused the quadriceps muscles,73,74 and recent studies highlight exercises incorporated into functional tasks.75–77 Most functional tasks involve the use of lower extremities, however it is often seen that women with PGP adapt to an inappropriate motor pattern where they, e.g. reduce using their lower extremities and compensate with the arms when standing up and sitting down on a chair. So, maybe the essential exercise for LBP and PGP is to primarily strengthen the lower extremities, thighs and buttocks? The quadriceps muscle exertion is the weak link for the squat technique74 and squats can be performed as home based exercises incorporated into functional tasks. Not all patients with LBP and PGP will however, benefit equally from exercises,78,79 hence patients should be encouraged to engage in regular exercises they personally enjoy with self-identified functional goals and meaningful movements.53
ConclusionIn conclusion, to increase from moderate to strong evidence of exercises, adherence of exercises is essential. To enhance adherence, exercises need to be meaningful to the patient, relevant for daily activities, individualized according to patient preferences, guided and supervised to secure performance and quality. Speak to the patient's heart and brain and tell them to practice what ‘they want to be good at, and no exercise is better than the way it is performed. Maybe, if mentioned aspects are taken into consideration, future randomized controlled trials will show strong effect of exercise programs for LBP and PGP.
Conflicts of interestThe author declares no conflicts of interest.
This paper is part of a Special Issue on Women's Health Physical Therapy.