In previous contributions to the Comprehensive Pain Management Editorial Series,1,2 we highlighted that stress (intolerance), in addition to sleep disturbances, also serves as an important perpetuating factor to many, if not all, patients with chronic pain, and has similar effects on immune health.3 Yet many clinicians feel uncomfortable dealing with stress (intolerance) in patients with chronic pain, leaving plenty of room to implement stress science in clinical practice. Therefore, this editorial will discuss the emerging role of stress (intolerance) and its management in patients with chronic pain.
Stress intolerance in chronic pain: the often neglected and undertreated perpetuatorStress is the continuous struggle of living organisms to preserve an internal dynamic state of equilibrium (i.e., homeostasis),4 and stress intolerance – often seen in patients with chronic pain - is the exacerbation or occurrence of symptoms (e.g., pain, fatigue, cognitive disturbances) in response to stress.5 Stressors can be any physical, psychosocial, or emotional factor that challenges homeostasis.4 Stress intolerance in patients with chronic pain can be explained by a dysfunctional physiological stress response system,6–12 which can involve either the short-term (i.e., sympathetic nervous system) or long-term (i.e., hypothalamus-pituitary-adrenal axis5) stress response system, or both (Fig. 1).
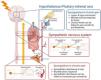
Dysfunctional stress systems in chronic pain. Stress activates the sympathetic nervous system (in red) and hypothalamus-pituitary-adrenal axis (in blue), resulting in the release of adrenaline, noradrenaline, and corticosteroids (e.g., cortisol). Both baseline activity as well as the response of both systems are abnormal in patients with chronic pain (reviewed in5).(For interpretation of the references to color in this figure legend, the reader is referred to the web version of this article).
A dysfunctional stress system can include a disbalance between the sympathetic and parasympathetic branches of the autonomic nervous system in favor of the former, which translates to sympathetic dominance at baseline indicating that the body is in a constant state of physical stress (possibly reflected in an increased in heart rate, blood pressure, or breathing rhythm; pupil dilatation; and sweating). The hypothalamus-pituitary-adrenal axis, illustrated in Fig. 1, is also activated in response to daily stressors, and plays a key role in recovering from stress (including physical activity) through its metabolic (raises blood glucose levels through gluconeogenesis13) and immune regulatory action (including a strong anti-inflammatory effect14). Unfortunately, the hypothalamus-pituitary-adrenal axis is dysfunctional in many patients with chronic pain, with observations ranging from hyper- to hypocortisolism.15,16 Moreover, the stress response, referring to the actual changes in activity of both the sympathetic nervous system and hypothalamus–pituitary–adrenal axis in response to stressors, is blunted in some chronic pain populations, implying the body is physically not capable of dealing with stressors accurately.5 Together, the sympathetic nervous system and the hypothalamus–pituitary–adrenal axis are the two main neural circuits through which our body adapts to stress. The brain regions responsible for top-down control of these ‘stress response systems’ frequently exhibiting altered functional behavior across various chronic pain populations,17–21 fitting well in our current understanding of chronic pain as a disease of the (central) nervous system.
Taken together, mounting evidence suggests that stress intolerance in patients with chronic pain can be explained by a dysfunctional physiological stress response system(s), conflicting with the common belief that stress (intolerance) is ‘in the mind’ and purely psychological in nature. This is important to explain to patients presenting with stress intolerance, as a more biopsychosocial understanding of their stress intolerance can be reassuring, and potentially can motivate them to engage in stress self-management strategies as explained below. In addition to the dysfunctional physiological stress response system, understanding the interplay between stress and the immune system can add to motivating clinicians and patients to take action and improve stress tolerance.
Stress and the immune systemStress is closely related to immune functioning and immune health, in a way that chronic stress induces immune dysregulation and a pro-inflammatory state.22 For instance, stress at work (e.g., overcommitment, effort-reward imbalance) is associated with poor immune functioning (e.g., reduced natural killer cell activity, reduced number of natural killer and T cell subsets), and increased inflammatory markers23,24 (Fig. 2). Moreover, chronic stress exposure results in accelerated immune aging.22,25,26 Such immune aging is characterized by an increased number of senescent T-lymphocytes, which show defects in proliferation and effector functions, and produce high amounts of proinflammatory cytokines.22,27 Immune aging also implies increased cellular aging, decreased responses to vaccines, and impaired control of latent viruses.22,26 These are remarkable findings underscoring the key role of stress tolerance in maintaining (or even restoring) immune health in all patients with chronic pain.
Improving stress tolerance in patients with chronic painFor patients with chronic pain and stress intolerance, clinicians can consider including stress management as an evidence-based28–30 component of an individually tailored, multimodal lifestyle intervention. Such stress management typically starts by educating the patient about the role of stress and its underlying mechanisms to broaden the patient's perceptions about stress intolerance (as explained above). In addition to stress education, stress management typically entails identification of relevant stressors and ‘uplifts’ (i.e., mood-uplifting activities), and teaching stress coping skills. The latter can include the Eliminate – Change – Accept (ECA) stress coping method. In this approach, patients reflect on the three options (eliminate – change – accept) for dealing with their stressors (explained in Table 1). This approach to stress coping also provides a framework for integrating relaxation skills (e.g., Jacobson progressive muscle relaxation, mindfulness, visualization, and breathing exercises) in the individually-tailored stress coping strategy.
The Eliminate – Change – Accept (ECA) method to cope with daily stress.
Another way of decreasing stress is by increasing greenspace exposure,31 which potentially can be combined with physical activity/exercise interventions. In addition, stress management can also include emphasizing a more positive view on stress management by facilitating (mood) uplifting activities and social support (Fig. 3). Low social support is common in patients with chronic pain,32,33 is often overlooked in chronic pain management,33 and implies more emotional distress and reduces stress tolerance.34 An evidence-based way of improving social support in patients with chronic pain include group-based interventions to creating a sense of community and belonging among patients.34 Social support can also be facilitated by proposing to the patient to bring a significant other (e.g., spouse, child, parent, friend) to the treatment sessions. This can be important for several reasons, including addressing the patient's feeling as though their friends and family do not believe that they have a ‘real’ condition, and sometimes even criticize, blame, or dismiss them, resulting in the feeling of invalidation.34,35 Engaging the significant other in selected components of the individually-tailored, multimodal lifestyle approach, such as pain science education and stress education/management, can improve the patient's social support and consequently stress resilience. This way, the significant other can become the patient's coach facilitating a healthy lifestyle outside the treatment sessions.
The third and final step of the individualized stress management approach for patients with chronic pain (Fig. 3) entails generalization from practicing relaxation exercises and stress-coping strategies (including enjoying mood uplifting activities, social support, and applying cognitive strategies) in a safe, relaxing environment towards a stressful situation. This can be achieved to gradually increasing the stressful nature of the situation in which the patient will practice the learned stress-coping strategy (i.e., from practicing in their bedroom with mobile phone in flight mode to practicing in a busy (living) room, during public transportation, and eventually prior, during, and/or following daily stressors). More details on how to provide stress management, including how to integrate it into exercise therapy, to patients with chronic pain is available elsewhere.36
Finally, stress management is not a separate entity or component but rather a continuity that runs through the entire individually-tailored, multimodal lifestyle intervention for patients with chronic pain.36 Accordingly, it should be considered that an unhealthy diet can serve as a stressor too, which in turn can decrease stress tolerance and increase pain sensitivity. Therefore, the next contribution to the Comprehensive Pain Management Editorial Series will address the emerging issue of diet, nutrition, and chronic pain (management).