Chronic pain, which must be understood as a complex biopsychosocial phenomenon, is strongly determined by the social and economic conditions in which people work and live. It is a global health problem that goes beyond individual suffering and represents a major public health challenge worldwide.1 The prevalence of chronic pain is alarming, affecting the quality of life of people across all ages and resulting in significant socio-economic burden in terms of healthcare utilization and loss of productivity.1 Additionally, the prescription of painkillers as the main policy strategy has led to opioid misuse and addiction so there is an urgent need to implement alternative non-pharmacological interventions for the management of persistent pain. In this context, physical therapy, which involves a variety of therapeutic interventions (e.g., exercise and education), has been shown to be effective in the management of chronic pain,2 in particular addressing the underlying physical, psychological, and social contributors to chronic pain.
Although physical therapy has been shown to be clinically and cost effective in the management of a wide variety of musculoskeletal disorders,3 access to these services remains unequal, leading to health inequalities that disproportionately affect vulnerable populations. In this sense, health democratization has been defined as achieving equity and universal access to quality health services, which requires genuine collaboration between health professionals, individuals, families, and communities.4 Democratizing access to physical therapy could contribute to breaking down the barriers that prevent people with chronic pain from seeking and receiving these services, thus ensuring equitable distribution. Consistent with previous recommendations for the democratization of health care,4 key strategies for democratizing access to physical therapy for people with chronic pain are described below.
Politics and cultureTo improve access to physical therapy for people with chronic pain, policies should promote coverage of physical therapy services, allocation of financial resources, equitable access, continuing education, and collaboration between different health professionals. In addition, health professionals and health policies should not overlook the influence of cultural factors on the experience of pain to ensure a patient-centered approach to treatment. Cultural diversity is reflected in beliefs, attitudes, and behaviors related to chronic pain, which poses important challenges in its clinical management.5 In this regard, promoting patient self-management and autonomy through active treatments (e.g., education and exercise) adapted to cultural diversity is key to the democratization of physical therapy.
Education and communicationEducation is a powerful tool to democratize access to health care and is considered a core component of the management of musculoskeletal pain.6 Education campaigns should focus on both people with chronic pain and healthcare professionals. Often, health professionals may overlook the importance of communication and the impact of words when delivering a medical diagnosis.7 For example, the word "degenerative" can be really alarming and lead to misinterpretation by patients, and an alternative term might be "normal age-related changes". Similarly, "chronic" could be replaced with "it may persist, but you can overcome it", while "instability" could be replaced with "needs more strength and control".7 Therefore, it is important to minimize the nocebo effect in clinical practice (e.g., verbal suggestions), as the magnitude of this effect on pain can be large.8 Additionally, failure to consider psychosocial factors such as catastrophizing or kinesiophobia, as well as the patient's educational level, may result in inadequate treatment, which in turn may limit the clinical outcomes. Although pain science education combined with exercise has been shown to be an effective strategy for reducing the perceived threat of pain and improving pain self-management,9 it often does not or only partially addresses the multiple lifestyle factors that may contribute to chronic pain (e.g. sleep disorders, unhealthy diet, smoking, stress, and sedentary lifestyle).10 Education programs should then identify and address barriers to behavioral lifestyle change and apply tailored interventions that facilitate long-term adherence.10 For example, physical therapists may provide sleep hygiene education as an entry point for sleep treatment.11
Raising community awareness of the benefits of physical therapy and healthy lifestyles through public health education initiatives could be critical in overcoming pain misconceptions, reconceptualizing pain, and promoting early active interventions. In addition, promoting a therapeutic alliance-centered approach, in which patients play an active role in the therapeutic process and the physical therapist acts as a facilitator or coach guiding patients toward their goals and managing their expectations, could improve adherence and long-term success in physical therapy programs. Therefore, physical therapists should receive training to improve their skills in active listening, individualized conversation, and empathy.
TechnologyUnprecedented access to the Internet and multimedia devices is changing the culture of physical therapy.12 A revolutionary approach to democratizing access to physical therapy could be the incorporation of telemedicine and digital platforms. Indeed, the effects of telerehabilitation have been shown to be comparable to those achieved with face-to-face rehabilitation or better than non-rehabilitation in different musculoskeletal pain conditions (e.g., osteoarthritis, low back pain, and hip replacement).13 Thus, remote rehabilitation and mobile apps can extend the reach of physical therapy to people living in rural areas and those with limited mobility or financial barriers. Also, the arrival of artificial intelligence (AI) through chatbots (e.g., ChatGPT, Google Bard) can also contribute to democratizing the access to education by managing recommendations for clinical practice and research.14
Social network and open scienceSocial networks offer a rapid method of dissemination, critical review, and potential application of research results, as well as reaching a wider range of potential end users (patients, clinicians, researchers, and policy makers).15 One recommendation to lend credibility to research disseminators using social networks is to provide a link to the original article (e.g., PubMed or equivalent) so that users can verify the results and assess their quality.15 Users should also be aware of the source of the information and any potential conflicts of interest. On the other hand, open science is a tool that facilitates access to reliable scientific research and provides a sound basis for informed decision-making about treatments for chronic pain. In addition, participation in virtual meetings and the use of videoconferencing platforms may facilitate the rapid dissemination of current approaches to chronic pain, thus greatly enhancing continuing education and improving the quality of care provided to patients.
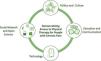
Integrating the four key elementsTo integrate these four key elements of democratization (Figure 1), it is essential that future studies evaluate the impact of implementing preventive programs based on effective coordination of several key strategies (Table 1) to ensure timely access to quality physical therapy. Promoting self-care and empowerment in people with chronic pain, who are generally (over) treated with the biomedical approach (e.g., use of analgesics) needs a paradigm shift. Democratizing access to physical therapy to address the public health challenge posed by chronic pain requires a comprehensive approach in line with current socio-cultural realities. This means that the vision must be dynamic and adaptable to each society and culture.
Main strategies to democratize access to physical therapy for people with chronic pain.
In conclusion, the coordination of political, cultural, educational, communicative, and technological strategies could contribute significantly to democratizing access to physical therapy and improving the quality of life of people with chronic pain. This paradigm shift could improve people's well-being, alleviate the burden on health systems, and contribute to a more equitable and sustainable future for patients, families, society, and the economy of countries.